The post Uterine Fibroids Treatment in Mumbai Know Symptoms, Causes, Risk Factors appeared first on Dr Sandhya Shah.
]]>Fibroids are also known as
- leiomyomas
- uterine myomas
- fibromas
- myomas
The Office on Women’s Health has reported that almost 80 percent of women are affected by the age of 50. But, most women don’t have any symptoms and may never even find out that they have fibroids.
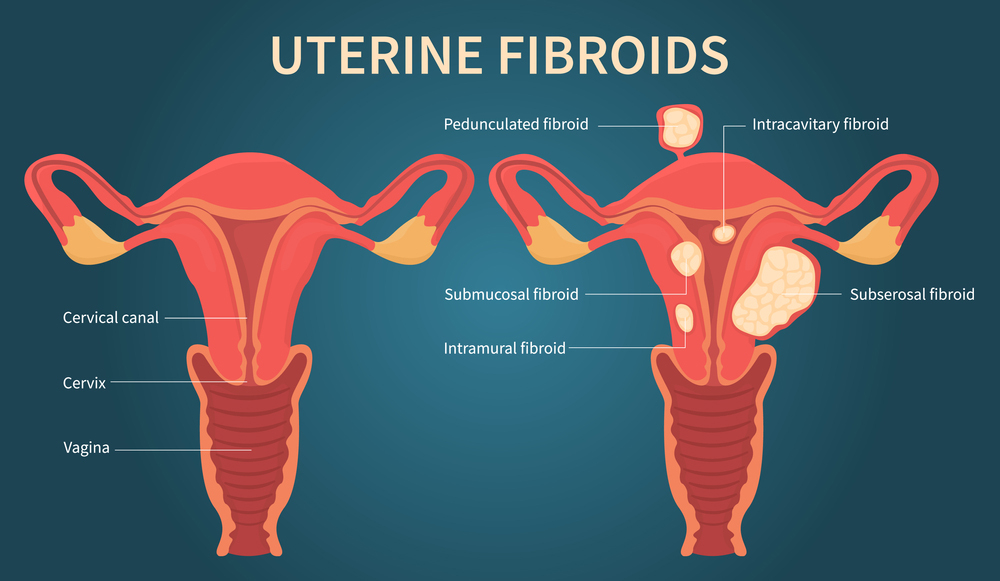
Who is at higher risk for Fibroids?
Women are at higher risk for acquiring fibroids if they have any of these risk factors:
- pregnancy
- age of 30 or older
- a high body weight
- a family history of fibroids
- African-American
Symptoms of Fibroids
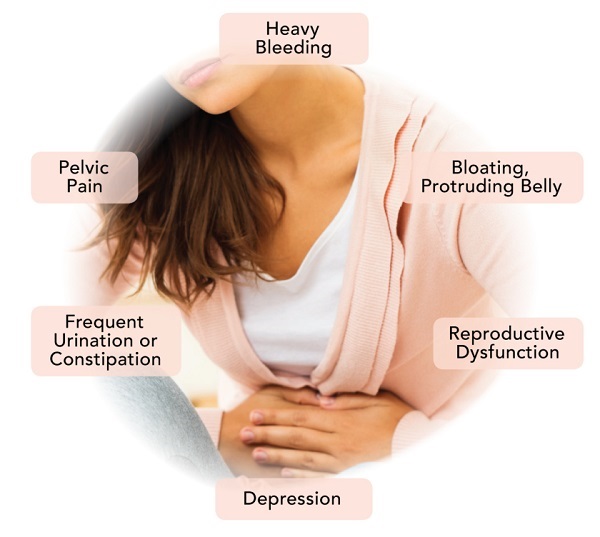
- Prolonged periods
- Bleeding between periods
- Pelvic pain
- Constant urination
- Lower back pain
- Pain during intercourse
- Difficulty getting pregnant
Your symptoms will also depend on the number of tumors you have and their location and size.
If your tumor is tiny or you’re undergoing menopause, you may not have witnessed any symptoms. Fibroids may shrink during and even after menopause. Women going through menopause are feeling a drop in their levels of progesterone and estrogen -hormones that stimulate fibroid growth.
Causes
- Many fibroids include changes in genes that vary from those in healthy uterine muscle cells.
- Estrogen and progesterone appear to encourage the growth of fibroids.
- Fibroids carry more estrogen and progesterone receptors than healthy uterine muscle cells do. Fibroids usually shrink after menopause because of a decrease in hormone production.
- Substances that support the body maintain tissues, for example, insulin-like growth factor, may influence fibroid growth.
- ECM (Extracellular matrix ) is the element that makes cells stick together. ECM is increased in fibroids and hence makes them fibrous. It also stores growth factors and creates biological changes in the cells themselves.
Treatment
Most fibroids do not require treatment. They usually disappear after menopause.
If fibroids cause uncomfortable symptoms, various medical treatments can help.
1] Medication
The first course of treatment for fibroids is Medication. Here are some possible medications in detail.
- Nonsteroidal anti-inflammatory drugs
Nonsteroidal anti-inflammatory drugs, for example, ibuprofen, can decrease fibroid pain but do not reduce bleeding.
- Hormonal birth control
Oral contraceptives can control the ovulation cycle and can help lessen the amount of bleeding during periods. A low dose of hormonal birth control will not make fibroids grow.
People use progesterone intrauterine devices or progesterone-like injections.
2] Surgery
Severe fibroids may not react to more conventional treatment options. In these instances, Surgery is the best option.
- Hysterectomy
It is the partial or complete removal of the uterus. This can treat extremely large fibroids or even excessive bleeding. Total hysterectomy can stop the return of fibroids.
If a surgeon removes the ovaries and fallopian tubes, side effects can include decreased libido and early menopause.
- Myomectomy
Removal of the fibroids from the muscular wall of the uterus is called Myomectomy. It helps people who want to have children.
Those with big fibroids or fibroids found in particular parts of the uterus may not profit from this type of Surgery.
- Endometrial ablation
Removing the uterine lining can help if fibroids are found near the inner surface of the uterus. This may be an efficient alternative to a hysterectomy for people with fibroids.
- Uterine fibroid embolization
Cutting the blood supply to the area contracts the fibroid. Led by fluoroscopic X-ray imaging, the doctor injects a chemical through a catheter inside the arteries, which supplies blood to any fibroids.
However, this method is not advised for women during pregnancy or for those who want to have children.
Furthermore, this is not a suitable treatment method for all types of fibroid.
3] Lifestyle changes
Keeping a moderate weight by regular exercise and eating a healthy diet may help moderate estrogen levels, which can help decrease fibroids.
Do’s and Dont’s
DO’S
- Load up on fresh fruits and vegetables
- Keep an eye on your blood pressure
- Manage your stress level
- Make yourself comfortable
- Discuss with your doctor before you experiment with any kind of supplement.
DONT’S
- Don’t eat a diet full of processed foods, red meats, and high-fat dairy
- Don’t skip your workouts.
- Don’t overdo it on the sugar
- Don’t smoke
Side-effects and risks after treatment
There can be risks. Medications do have side effects, and few may not be good for you. Speak to your healthcare provider about the medications you are taking for other medical conditions and your medical history before beginning with a new medication.
There are also risks associated with the surgical treatment of fibroids. Any surgery will place you at risk of infection, bleeding, or any natural risks because of Surgery and anesthesia. An extra risk of fibroid removal surgery includes future pregnancies. Some surgical options can stop future pregnancies. Myomectomy is a procedure that will only remove the fibroids, allowing for future pregnancies. Though, women who have had a myomectomy may need to deliver future babies by Caesarean section.
Uterine fibroids are a normal condition that several women face during their life. In few cases, fibroids are small and hence don’t cause any symptoms at all. But at other times, fibroids can cause uncomfortable symptoms. Fibroids can indeed be treated, and, usually, your symptoms can be improved.
Frequently Asked Question and Answers
1. Can fibroids be treated without surgery ?
According to WebMD the non surgical treatment of fibroids is possible using medication or through Uterine Fibroid Embolization (UFE).
The post Uterine Fibroids Treatment in Mumbai Know Symptoms, Causes, Risk Factors appeared first on Dr Sandhya Shah.
]]>The post Important Things About Maintaining the High-Risk Pregnancy appeared first on Dr Sandhya Shah.
]]>Reasons that a pregnancy can be treated as a high-risk one:
Maternal age: The pregnant woman’s age is a common risk factor for high-risk pregnancies. Women under 17 years or over the age of 35 will experience additional difficulties. If a woman is conceiving after the age of 40, there is also a chance of miscarriage and the possibility of genetic problems.
Health issues that existed before being pregnant, such as heart issues, renal issues, diabetes, high blood pressure, STDs, or chronic illnesses like HIV, might increase the risk for both the mother and the unborn child. Issues from previous pregnancies or a history of miscarriages are also risk factors for the pregnancy’s higher risks. Before planning to conceive, it is best to speak with a doctor specializing in high-risk pregnancies in Indore. To avoid any adverse effects throughout your pregnancy, your doctor will run specific tests, modify your medications, and provide recommendations for safety precautions you may take.
To prevent pregnancy complications:
Even if you are in good health, your doctor may encourage you to schedule a check-up to improve your health before becoming pregnant. You will be requested to consider a few measures to avoid various risks. Some of them are:
- Take appropriate vaccines.
- Get 400 mg of folic acid daily before and after conception.
- Maintain a healthy weight by eating well.
- Avoid using tobacco, alcohol, narcotics, and other dangerous substances since doing so puts you and your unborn child in danger.
- Consult your obstetrician as soon as possible and discuss any issues you have while pregnant.
Take away:
Your High-Risk Pregnancy Doctors in Indore may advise you to contact a primatologist if your pregnancy has a higher risk. You will receive assistance from an obstetrician who has received specialized training in treating high-risk pregnancies. This specialist will collaborate with other experts to ensure you get the best outcomes possible for you and your kid.
The post Important Things About Maintaining the High-Risk Pregnancy appeared first on Dr Sandhya Shah.
]]>The post Management of Ectopic Pregnancy: What Every Woman Should Know appeared first on Dr Sandhya Shah.
]]>One potentially fatal side effect of pregnancy is ectopic pregnancy. It happens in 2 to 5 occurrences out of every 1,000 pregnancies and occurs when the fertilized egg implants outside the uterus.
Older age, heavy menstrual cycles, obesity, having several sexual partners, and being underweight raise the chance of ectopic pregnancy.
Women who have experienced one ectopic pregnancy may be more likely to do so again.
The following are the most typical symptoms of ectopic pregnancy; if you experience any, you should consult your doctor first:
- Pain in the pelvis, lower abdomen, or area below the belly button.
- Bleeding from the cervix, typically a brownish discharge.
- Nausea, discomfort, abdominal swelling, and vomiting
The first few weeks are when these symptoms are most prevalent. Blood clots typically form in the fallopian tubes after two to three months. Compared to a typical intrauterine pregnancy, your odds of delivering the baby to term are much reduced. The most hazardous consequence following an ectopic pregnancy is shock and a higher chance of infertility.
Some of the common treatments for ectopic pregnancy are:
- Medications: A typical pregnancy’s medical care is comparable to an ectopic pregnancy. Antibiotics are frequently administered because they can reduce the risk of miscarriage. Progesterone supplements and pelvic rest are effective treatments for women who haven’t previously experienced an ectopic pregnancy. Mifepristone, a medication that aids in the fallopian tube’s emptying, is occasionally paired with pelvic rest.
- Surgery: Another solution is to have a laparoscopic procedure. A tiny tube known as a cannula is inserted into the stomach to access the cervix during the procedure. The ectopic pregnancy can be removed in a less harmful and painful manner.
- Tubal ligation or salpingectomy: A tubal ligation is the last available alternative. A surgeon will cut open the fallopian tube and remove the embryo from the uterus. Although it’s doubtful that you’ll become pregnant following this operation, there might be major problems if you do.
Conclusion
Although it can happen to anybody, ectopic pregnancies most frequently affect women between the ages of 15 and 24. If this ailment is not addressed immediately, it might be hazardous. If the developing embryo is not attended to, it may burst, resulting in excessive bleeding, sterility, and other problems. To avoid serious consequences from a ruptured ectopic pregnancy, you should visit your gynecologist expert in Indore as soon as possible if you have an ectopic pregnancy.
The post Management of Ectopic Pregnancy: What Every Woman Should Know appeared first on Dr Sandhya Shah.
]]>The post Why Minimally Invasive Surgery Might Be Necessary for Your Endometriosis? appeared first on Dr Sandhya Shah.
]]>What is Endometriosis?
Endometriosis is a disorder in whic, the tissue that typically lines your uterus – the endometrium, begins to develop outside of it. Studies estimate the number of women affected at 176 million. Women’s reproductive health may suffer uncomfortable and negative impacts from this illness.
What are the causes?
Endometriosis’s root cause is yet unknown. However, studies have connected some characteristics, such as getting your first period at a young age and having endometriosis in your family, to an increased chance of developing the condition. Additionally, there is some evidence that some fertility treatments may raise your risk, but most medical professionals believe that using these drugs does not guarantee the development of endometriosis.
What are the diagnostic methods?
You should make book an appointment with your doctor if you suspect that you have endometriosis. They will inquire about your signs and symptoms and perform a pelvic examination. They will suggest you to a specialist who can do minimally invasive surgery (laparoscopic surgery) to diagnose endometriosis if they think you might have it. Your doctor will make a tiny incision in your lower belly and use a small telescope to do laparoscopic surgery.
Laparoscopic surgery for endometriosis
Endometriosis is a condition that is increasingly being treated using minimally invasive surgery. This is because minimally invasive surgery is less intrusive. It is also because this operation has such high success rates. It is also a brilliant option for ladies who are done having children. However, the procedure combines a laparoscopy, making it somewhat invasive. During a laparoscopy, the endometriosis is visible to the doctor. The doctor can remove the tissue if the condition is severe and hurting. The doctor could decide to ignore endometriosis if it is not hurting.
Hysterectomy can be performed as part of the operation or separately. In addition to the uterus, the cervix, ovaries, fallopian tubes, and surrounding tissue may be removed during a hysterectomy. Most of the time, the doctor leaves the vagina intact. Total abdominal hysterectomy with salpingo-oophorectomy is the medical term for this treatment. A woman who undergoes a hysterectomy and has her ovaries removed develops menopause immediately.
The post Why Minimally Invasive Surgery Might Be Necessary for Your Endometriosis? appeared first on Dr Sandhya Shah.
]]>The post Uterine Inflammation: Causes, Symptoms, Treatment Options appeared first on Dr Sandhya Shah.
]]>White blood cells, cytokines, and inflammatory mediators are released into the uterine fluid during an immune response that results in uterine inflammation, also known as endometritis or endometrium.Most frequently, this happens with bacterial infections after parturition (childbirth), miscarriage, induced abortion, IUD usage, and the presence of an ongoing genital tract infection. Fever, discomfort, and uterine contractions may also result from it.
What are the causes?
Germs frequently bring on uterine infection. Streptococcus, staphylococcus, listeria, and clostridium are some of the most typical bacteria that cause uterine infections. Sometimes a chemotherapy-related inflammation of the uterus can be brought on by a chemotherapeutic drug like mitomycin or doxorubicin, which is often used to treat cancer. A virus or fungus may also be the source of a uterine infection.
What are the symptoms?
Fever, chills, vaginal discharge with an unpleasant odor, uterine cramps, and maybe scarring of the uterus are all indications of active uterine inflammation.
What are the diagnostic methods?
The doctor will analyze your medical history, clinical information (including signs and symptoms), physical exam results, and laboratory testing to diagnose uterine inflammation correctly. The doctor often conducts a pelvic exam to determine the pathologic cause of the uterine infection.
What are the treatment methods?
The intensity of uterine inflammation determines the course of therapy. Oral antibiotics can be used to treat a minor disease case at home. Two different antibiotics may occasionally be prescribed by a doctor to be taken concurrently yet independently. The uterine infection may occasionally be treated with intravenous (IV) antibiotics.
What are the preventive measures?
Maintaining good hygiene and thoroughly cleansing oneself after any activity can reduce your risk of developing uterine irritation. To relieve the itching, burning, or pain in your vagina, you can use an over-the-counter vaginal cream, pills, or combination treatments. Avoid introducing anything into the vagina, including your fingers and tampons, and avoid douching as this might increase your risk of infection.
Take Away
Although uterine inflammation occurs abruptly and is not cause for concern, if you have a fever or other infection-related symptoms, call your doctor right once.
The post Uterine Inflammation: Causes, Symptoms, Treatment Options appeared first on Dr Sandhya Shah.
]]>The post Ovarian cysts: All you need to know appeared first on Dr Sandhya Shah.
]]>Several women have ovarian cysts. Most ovarian cysts display little or no discomfort and are considered harmless. The majority vanishes without treatment within few months.
However, ovarian cysts that have ruptured can cause severe symptoms. To protect your health, get routine pelvic exams and identify the symptoms that can indicate a serious problem.
Types of Ovarian cysts
The two types of ovarian cyst are:
- Functional ovarian cysts develop as a part of the menstrual cycle and are normally harmless and short-lived.
- Pathological ovarian cysts develop as a result of abnormal cell growth; these are much less common.
Symptoms
An ovarian cyst usually causes symptoms if it splits, is huge, or prevents the ovaries’ blood supply.
- Pelvic pain – It can cause a heavy sensation to a severe and sharp pain.
- Pain during sexual intercourse
- Difficulty clearing your bowels
- A frequent urge to urinate
- Heavy, irregular, or lighter periods than usual
- Swollen tummy
- Difficulty getting pregnant
Symptoms of a ruptured ovarian cyst
A ruptured ovarian cyst will not always produce symptoms, especially if the cyst is small. Though, sometimes a ruptured ovarian cyst can lead to pain and internal bleeding. The pain typically comes on suddenly and occurs only on one side. The pain may occur during physical activity or sexual intercourse. A ruptured ovarian cyst normally does not cause fever or gastrointestinal symptoms.
How are Ovarian cysts diagnosed?
Sometimes ovarian cysts can be seen by a doctor during a bimanual examination of the pelvis. If a cyst is speculated based on symptoms or physical examination, imaging techniques are applied. Most cysts can be diagnosed by ultrasound, which is the ideal imaging technique for identifying them. Ultrasound makes use of sound waves to get an image of structures inside the body. Ultrasound imaging is painless and does not cause any harm. Transvaginal ultrasound is a diagnostic tool to visualize the ovaries using a thin ultrasound probe in the vagina.
Causes of Ovarian cysts
Most ovarian cysts occur due to your menstrual cycle. Other types of cysts are less common.
Functional cysts
Your ovaries usually grow structures called follicles every month. Follicles generate the hormones (estrogen and progesterone) and release an egg whenever you ovulate.
If a regular monthly follicle keeps growing, it’s known as a functional cyst. There are two different kinds of functional cysts:
- Follicular cyst-Around the midpoint of your menstrual cycle, the egg rushes out of its follicle and goes down the fallopian tube. A follicular cyst occurs when the follicle doesn’t rupture or release the egg but proceeds to grow.
- Corpus luteum cyst-When a follicle releases the egg, it starts producing the hormones estrogen and progesterone for conception. This follicle is called the corpus luteum. Fluid can accumulate inside the follicle, prompting the corpus luteum to grow into a cyst.
Functional cysts are known to be harmless and often disappear on their own.
Other cysts
Cysts not linked to the normal function of your menstrual cycle
- Dermoid cysts-Called as teratomas, these cysts contain tissue, such as hair, skin, or teeth, as they form from embryonic cells.
- Cystadenomas- They develop on the surface of the ovary and might be filled with a mucous material.
- Endometriomas-These grows as a result of a condition in which uterine endometrial cells develop outside your uterus. Some of these tissues can attach to your ovary and create growth.
Dermoid cysts and cystadenomas can grow large, causing the ovary to move out of its position. This raises the chance of painful twisting of your ovary, which is called ovarian torsion. Ovarian torsion can also result in decreasing or even stopping the blood flow to the ovary.
Treatment
Most ovarian cysts disappear naturally in about one to three months, although they can rupture and create pain. They are harmless and have no long-term consequences. All women will have follicular cysts at some point that can go unnoticed.
Ultrasound is helpful to determine if the cyst is simple or compound.
In summary, the perfect treatment of ovarian cysts depends on the cause of the cysts and if it is producing symptoms or not. The age, the cyst’s size, and the cyst’s features on ultrasound are also factors that help decide the treatment. Cysts that are functional are observed with regular monitoring unless they rupture and cause bleeding, in which case surgical treatment is needed. Benign and malignant tumors need an operation.
Treatment can be simple observation, or it can even involve evaluating blood tests such as a CA-125 to determine the potential for cancer.
There are no home remedies to cure ovarian cysts other than taking non-steroidal anti-inflammatory drugs only for pain management.
Surgery for Ovarian cysts
The cyst can be surgically removed with laparoscopy, or if required, an open abdominal incision, i.e., laparotomy, if it is causing extreme pain. After the cyst is removed, the growth will be sent to a pathologist who studies the tissue under a microscope to make a conclusive diagnosis as to the type of cyst.
Which specialties of doctors can treat ovarian cysts?
Gynecologists-obstetricians are the medical specialists that can treat ovarian cysts.
Prevention
Although there’s no proven way for the prevention of ovarian cysts, regular pelvic exams can help guarantee that changes in your ovaries are diagnosed as soon as possible. Stay alert to changes in your monthly cycle, like unusual menstrual symptoms, particularly the ones that endure for more than a few cycles.
The post Ovarian cysts: All you need to know appeared first on Dr Sandhya Shah.
]]>